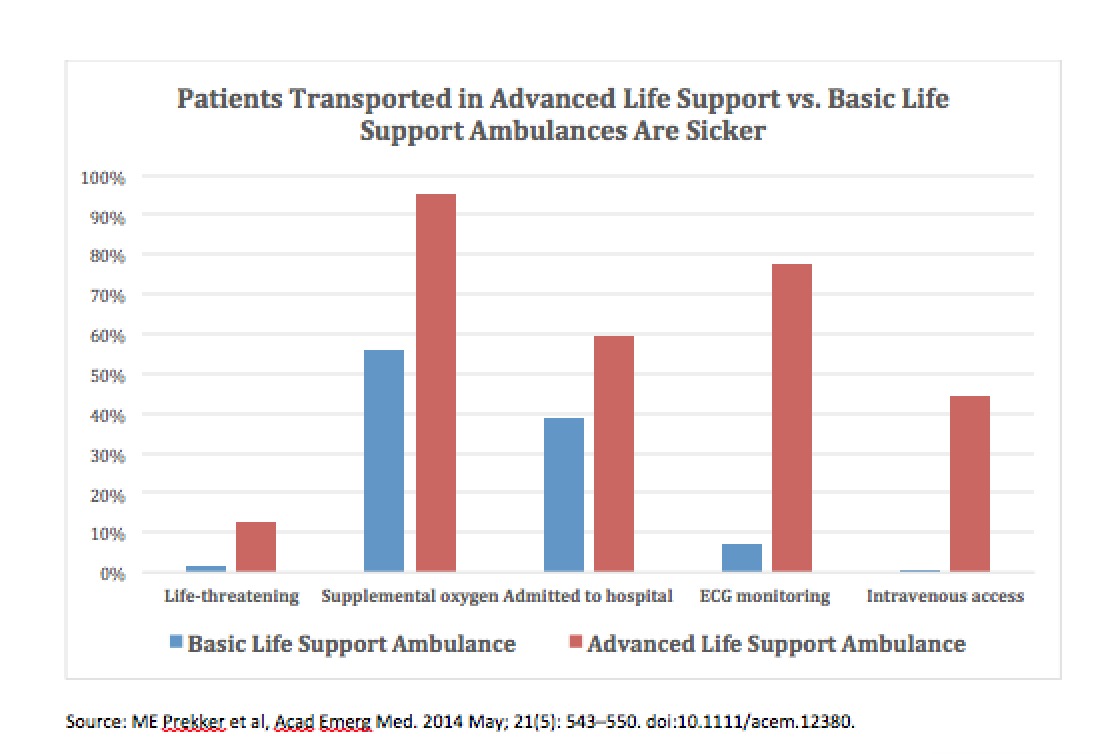
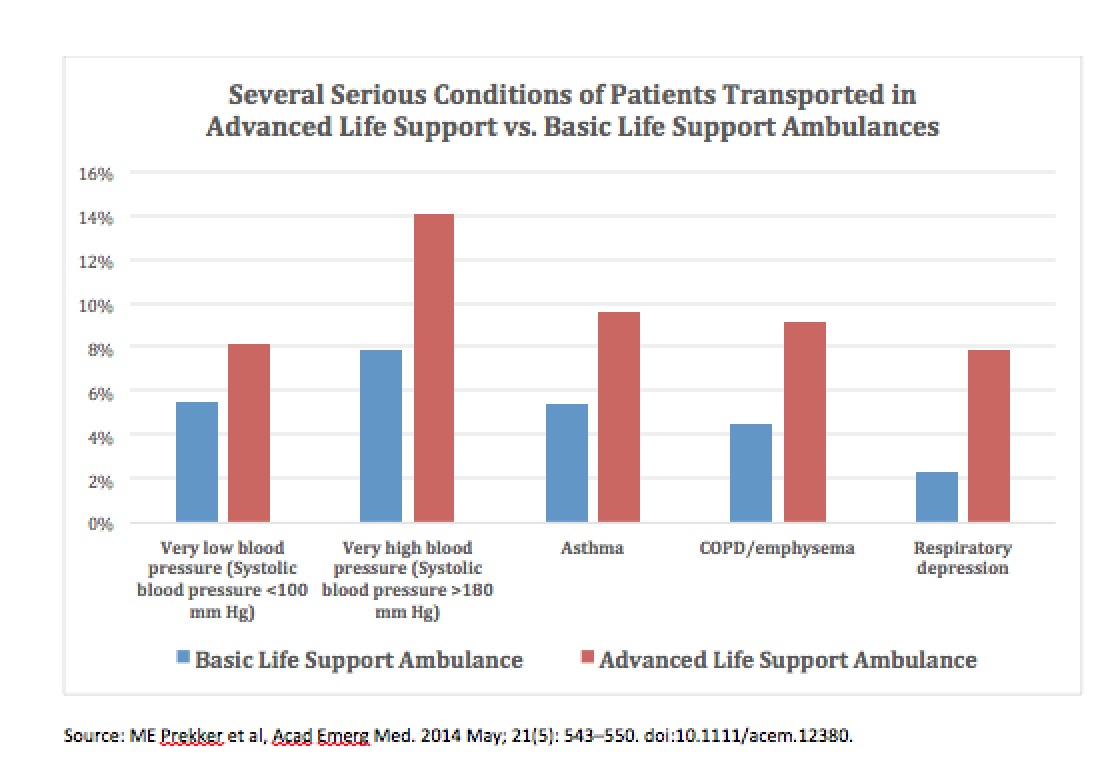
You can find the full text of the Senate Bill here.
Following is the Senate Republicans summary of their Obamacare replacement bill, with comments by NYU’s Jason Chung.
Seven years ago, Democrats imposed a risky health care experiment on Americans that led to skyrocketing costs and collapsing insurance markets. Senate Republicans are working to fix the mess Democrats made by acting to rescue the millions trapped by Obamacare.
Jason Chung: While Obamacare has been largely successful in its aims to get millions of uninsured Americans medical coverage, including low-income and those with pre-existing conditions, it has also thus far failed to rein in premiums. Some of that can be attributed to Obamacare failing to institute a public option, which would charge premium lower by 7% to 8% according to the Congressional Budget Office.
This is a nuanced position. One can support former President Obama for extending coverage for up to 17.7 million more people and criticize him for failing to account for or communicate the possibility of rising premiums in an unchecked for-profit health insurance model.
The discussion draft will:
Help stabilize collapsing insurance markets that have left millions of Americans with no options.
Jason Chung: As noted by the New York Times, Obamacare failed to create competition in the insurance marketplace but it didn’t create the lack of options that already existed.
Free the American people from the onerous Obamacare mandates that require them to purchase insurance they don’t want or can’t afford.
Jason Chung: Though the individual mandate was one of the least popular elements of Obamacare, it still had the support of 50% of those polled in March 2017.
http://www.cnn.com/2017/03/07/politics/health-care-replacement-poll/index.html
It’s noteworthy that the individual mandate was actually the creation of conservative economist, Mark Pauly, to solve the free rider problem
https://www.washingtonpost.com/blogs/ezra-klein/post/there-was-a-reason-conservatives-once-supported-the-individual-mandate/2012/03/30/gIQAiddnlS_blog.html
Without a single payer option, it is notable that any individual mandate will have difficulties as some people will simply not comply with the law or have coverage that is too low as the Cato Institute notes.
https://www.cato.org/blog/two-reasons-why-individual-mandate-will-not-solve-free-rider-problem
Improve the affordability of health insurance, which keeps getting more expensive under Obamacare.
Jason Chung: The draft bill includes the sunset of “Essential Health Benefits” as per s. 126(b). These benefits currently ensure that health insurance includes items that make having health insurance worthwhile such as:
– Outpatient care
– Emergency room trips
– In-hospital care
– Pregnancy, maternity and newborn care
– And more…
http://www.nbcnews.com/health/health-care/gop-health-care-debate-what-are-essential-benefits-n737646
Dropping these provisions would bring down the costs of basic premiums but also ensure that the most basic coverage is saddled with unaffordable co-pays and deductibles for those least likely to be able to afford them.
Preserve access to care for Americans with pre-existing conditions, and allow children to stay on their parents’ health insurance through age 26.
Jason Chung: This was a key promise made by then-candidate Trump to 60 Minutes on the campaign trail. He admitted at the time that this would “add costs”.
https://www.forbes.com/sites/brucejapsen/2016/11/20/trumps-epiphany-to-let-young-adults-stay-on-their-parents-insurance/#163538357423
Strengthen Medicaid for those who need it most by giving states more flexibility while ensuring that those who rely on this program won’t have the rug pulled out from under them.
Jason Chung: States would have more flexibility but the impact is unclear.
Currently, Medicaid funds all needs of patients but the new s. 1903B states that starting 2020 states will have to choose between a capped block grant or a capped amount per capita.
Overview of the Discussion Draft of Senate Amendment to H.R. 1628
Help stabilize collapsing insurance markets that have left millions of Americans with no options.
Short-Term Stabilization Fund: To help balance premium costs and promote more choice in insurance markets throughout the country, this stabilization fund would help address coverage and access disruption – providing $15 billion per year in 2018 and 2019; $10 billion per year in 2020 and 2021.
Jason Chung writes: S. 106(h)(1) specifies that these amounts are intended to “fund arrangements with health insurance issuers to address coverage and access disruption…” Rand Paul opposes this fund as an example of “new entitlements”.
http://thehill.com/homenews/senate/339008-four-senate-conservatives-say-they-oppose-obamacare-repeal-bill
Cost-Sharing Reductions: Continues federal assistance – through 2019 – to help lower health care costs for low-income Americans in the individual market.
Jason Chung writes:
Ensured by s. 207 but s. 208 explicitly repeals the cost-sharing subsidy after 2019.
Extending the subsidy but eliminating penalties is described as “a contradiction in many ways” by Michael Dowling, the CEO of Northwell Health. He points out that subsidies will now have to be substantial to attract people.
https://www.usatoday.com/story/news/politics/2017/06/22/keeping-money-insurance-subsidies-gop-health-bill-may-lower-premiums/103102580/
Free the American people from the onerous Obamacare mandates that require them to purchase insurance they don’t want or can’t afford.
Repeals the individual and employer mandates.
Improve the affordability of health insurance, which keeps getting more expensive under Obamacare.
Long-Term State Innovation Fund: Dedicates $62 billion, over 8 years, to encourage states to assist high-cost and low-income individuals to purchase health insurance by making it more affordable.
Tax Credits: Targeted tax credits will help defray the cost of purchasing insurance; these advanceable and refundable credits – adjusted for income, age and geography – will help ensure those who truly need financial assistance can afford a health plan.
Jason Chung: Eligibility for the premium tax credit will be reduced from those making 400 percent of the poverty line to 350 percent, as per s. 102(a)(1)(A). But, as the Atlantic notes, the poor and near poor would probably fare slightly better under this regime.
https://www.theatlantic.com/politics/archive/2017/06/ahca-senate-draft-medicaid-changes/531231/
Health Savings Accounts: Expanded tax-free Health Savings Accounts to give Americans greater flexibility and control over medical costs; increased contribution limits to help pay for out-of-pocket health costs and to help pay for over-the-counter medications.
Repeals Obamacare Taxes: Repeal costly Obamacare taxes that contribute to premium increases and hurt life-saving health care innovation, like the taxes on health insurance, prescription drugs, medical devices, and “high-cost” employer sponsored plans.
Jason Chung: The Democrats are sure to focus on ss. 112 and 113 which repeals taxes on pharmaceuticals and medical device
companies – two constituencies not exactly popular with the public at the moment.
https://fivethirtyeight.com/features/republicans-obamacare-repeal-would-cut-taxes-but-mostly-in-blue-states/
Oddly, s. 118 repeals the tanning tax despite the usage of tanning salons leading to increases in rates of melanoma, basal cell carcinoma and squamous cell carcinoma.
https://www.cdc.gov/cancer/skin/basic_info/indoor_tanning.htm
Senator Bob Casey (D- PA), highlights this “without comment”.
Page 29. This one I submit without comment. pic.twitter.com/YlQiEkCHd9
— Senator Bob Casey (@SenBobCasey) June 22, 2017
Empowers states through state innovation waivers (Obamacare 1332 Waiver): Provide states additional flexibility to use waivers that exist in current law to decide the rules of insurance and ultimately better allow customers to buy the health insurance they want. Allow the Department of Health and Human Services (HHS) to fast-track applications from states experiencing an Obamacare emergency.
Jason Chung: 1332 waivers allow states to develop innovative solutions for their individual health care markets. Hawaii’s application was the first in the nation to be approved.
https://www.cms.gov/CCIIO/Programs-and-Initiatives/State-Innovation-Waivers/Downloads/Hawaii-1332-Letter-final-and-signed.pdf
It remains to be seen how Republicans will react if 1332 waivers are used to push through single-payer health care in certain states.
http://www.newsweek.com/public-option-healthcare-slipping-through-back-door-498413
Preserve access to care for Americans with pre-existing conditions, and allow children to stay on their parents’ health insurance through age 26. (There are no changes to current law as it applies to Veterans, Medicare, or Social Security benefits.)
Jason Chung: S. 202 provides states with $2,000,000,000 in grants for fiscal year 2018. But this may be a one-off handout as it has no apparent mechanism for renewal.
Strengthen Medicaid for those who need it most by giving states more flexibility while ensuring that those who rely on this program won’t have the rug pulled out from under them.
Targets Medicaid to Those Most in Need: In 2021, begins gradual reductions in the amount of federal Obamacare funds provided to expand Medicaid, restoring levels of federal support to preexisting law by 2024 while providing fairness for non-expansion states.
New Protection for the Most Vulnerable: Guarantees children with medically complex disabilities will continue to be covered.
Provides additional state flexibility to address the substance abuse and mental health crisis.
Flexibilities for Governors: Allows states to choose between block grant and per-capita support for their Medicaid population beginning in 2020, with a flexibility in the calculation of the base year. Allows states to impose a work requirement on non-pregnant, non-disabled, non-elderly individuals receiving Medicaid.
New Protections for Taxpayers: Curbs Medicaid funding gimmicks that drive up federal costs.